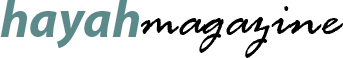To avoid a frantic race to the restroom, people with ulcerative colitis (UC) often struggle to decide what to eat for lunch. Although there is no specific diet for ulcerative colitis, many flare-ups of the disease can be controlled with the use of medicine and a healthy eating plan.
What is Ulcerative Colitis?
Like Crohn’s disease and microscopic colitis, ulcerative colitis is a form of IBD that affects the colon and lasts for an extended period of time (large intestine).
Health experts have estimated that 2 million people around the world suffer from IBD.
Inflammation and ulcers in the gut lining are symptoms of ulcerative colitis. The rectum is often the site of the first inflammation, although the entire large intestine is not immune to infection.
Does changing your diet make a difference?
Although nutrition does not cause UC, it can help manage symptoms like diarrhea during flares and keep you in good health overall. With time, you may learn that a select few foods bring on a flare-up of your UC symptoms and should be avoided. But, avoid cutting out entire food groups if you’re worried about missing out on essential nutrients.
Ulcerative colitis: what to eat and what not to eat
Although there is no “cure-all” diet for ulcerative colitis, avoiding items that are known to aggravate symptoms can assist.
Foods to eat
The general consensus amongst medical professionals is that those with UC should try to consume a balanced diet on a regular basis.
Those with ulcerative colitis may benefit from eating foods like:
- Foods high in omega-3 fatty acids: Some evidence suggests that eating foods rich in omega-3 fatty acids, like salmon, mackerel, walnuts, flaxseed, hemp, and chia seeds, can help persons with ulcerative colitis. The inflammatory bowel disease community can benefit from eating more of these foods, according to the IOIBD.
- Some probiotic foods: Yogurts, which are a good source of live probiotic cultures, fall into this category. This may help with digestion because of the “healthy” bacteria contained therein. Regular use of probiotics has been demonstrated to lessen the severity of flare-ups and other symptoms of ulcerative colitis.
- Fruits low in fiber: For those with ulcerative colitis, fruits like bananas, cantaloupes, and prepared fruits may be an option.
- Refined grains: They may be more digestible than whole grains. White potatoes, white pasta, white rice, white bread, and oatmeal are all examples. Most white bread and other grain products now come with added vitamins and minerals thanks to this practice.
- Lean protein: A person with ulcerative colitis may benefit from consuming protein sources other than red meat. They can range from hard tofu to fish and poultry to eggs.
- Vegetables: those with ulcerative colitis may be able to eat cooked veggies without the peel if the vegetables aren’t cruciferous. Vegetables such as cukes, squash, and asparagus spears fall into this category.
- More fluids: Diarrhea can cause dehydration, so people with illnesses like ulcerative colitis may need to drink more water than usual.
- Dietary supplements: Protein shakes and oral vitamin supplements may help patients with ulcerative colitis acquire the nutrients they need.

Food items to limit
To see what you should not eat if you have ulcerative colitis, look here. You should limit your intake of acidic and spicy foods, as well as coffee and other carbonated beverages
Caffeinated and decaffeinated coffee and tea both accelerate acid production and can lead to indigestion, especially for people who already suffer from stomach ulcers. Besides this avoid taking these food items:
- Alcohol: Due to the risk of bleeding and inflammation, people with stomach ulcers should avoid alcohol.
- Hot and acidic foods: Acid reflux is linked to stomach ulcers, thus it’s necessary to take precautions when eating these foods. The symptoms of stomach ulcers might be made worse by these foods since they increase stomach acid and can even cause acid reflux.
- Additional foods: Some of the best doctors advise minimizing consumption of refined foods such as white bread, pasta, and sugar; red meats; and trans fats present in commercially baked items and processed foods in addition to caffeine, alcohol, and carbonated drinks.
Other tips
If you have UC, here are some easy guidelines to follow when it comes to what you eat:
- Instead of having three large meals a day, divide them up into four or six smaller ones.
- Avoid gulping your food and instead chew it thoroughly.
- Track your food intake each day by keeping a food journal. In order to ensure that you get the proper amount of nutrients and calories each day, there are apps available to assist you in doing so.
- Drink plenty of water to stay hydrated.
- Avoid using straws, as swallowing air through them can lead to uncomfortable gas and bloating.
Adverse effects
When you change your eating habits, your body may need time to adjust. Your bowel habits may shift if, for instance, you begin eating more or less fiber.
Tell your doctor if you feel these symptoms aren’t getting better or are worsening. Constipation can develop in those who consume too little fiber. If you have a persistent digestive condition, you should report any changes in bowel motions to your doctor, who may recommend simple solutions like increasing your water intake or taking a fiber supplement.
Conclusion
Long-term, chronic UC can lead to intestinal inflammation and digestive problems. Dietary changes are often helpful in managing UC symptoms and even triggering remission for some people.
The best strategy to reduce your specific symptoms is to keep a food diary to record which foods you can and cannot eat and to maintain regular communication with your doctor to make sure you’re getting the right nutritional balance in your diet.
1. Is there a list of foods that can help fight against ulcerative colitis?
Some persons who suffer from UC may be able to stave off the onset of symptoms by eating a diet high in peeled fruits, cooked low-fiber vegetables, lean meats, and seafood.
2. Does ulcerative colitis get worse when you eat certain foods?
Symptoms of ulcerative colitis can be made worse by consuming foods heavy in insoluble fiber, lactose, and sweets.
3. What is the most effective protein for ulcerative colitis?
During an IBD flare, lean, skinless, boneless chicken breast is a great protein source. Meat contains saturated fat, which some studies have linked to inflammation.